Malnutrition in the elderly, particularly those in care homes, is a significant concern and can have a wide range of effects on their health and well-being. Here are a few key areas that malnutrition can affect:
- Immune System: Malnutrition can weaken the immune system, making the elderly more susceptible to infections and illnesses. This is particularly concerning in a care home setting where infections can spread more easily.
- Muscle Weakness and Mobility Issues: Inadequate nutrition can lead to muscle weakness, making it difficult for the elderly to perform daily activities. This can also increase the risk of falls and related injuries.
- Bone Health: Malnutrition, especially a deficiency in calcium and vitamin D, can contribute to weaker bones and increase the risk of fractures and osteoporosis.
- Wound Healing: Poor nutrition can slow down the healing process of wounds. In the elderly, this can be particularly problematic for those with chronic conditions like diabetes or for those recovering from surgery or injuries.
- Mental Health: There is a link between nutrition and mental health. Malnutrition can exacerbate symptoms of depression and anxiety and can also affect cognitive functions, leading to issues like confusion and memory loss.
- Overall Health and Quality of Life: Malnutrition can impact the overall health of elderly individuals, leading to a general decline in their quality of life. It can make them more lethargic, less able to enjoy activities, and more dependent on others for care.
- Increased Healthcare Needs: Malnourished elderly individuals often require more medical interventions and have longer recovery times from illnesses and surgeries. This can increase healthcare costs and the need for more intensive care.
Care homes need to have effective nutritional programs in place to prevent and address malnutrition among their residents. This involves not only providing nutritious meals but also monitoring the nutritional intake and health of each resident.
The best guidance is for the elderly to follow the eatwell guide produced by the government.
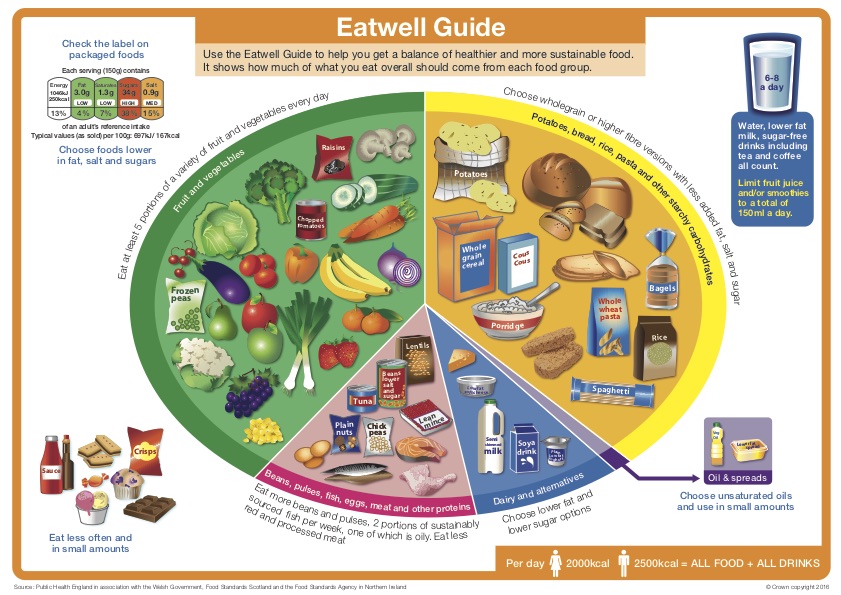
The NHS has produced this set of guidelines for nutritional care. You can download a poster from the NACC and learn more on their website. More comprehensive information is available in the publication Nutritional Standards for Adults, available from the NACC.
10 Key characteristics for good nutritional care
1. Everyone using healthcare and care services is screened to identify those who are malnourished or at risk of becoming malnourished.
2. Everyone using care services has a personal care support plan and where possible have had personal input, to identify their nutritional care and fluid needs and how they are to be met.
3. The care provider must include specific guidance on food and beverage services and nutritional care in its service delivery and accountability arrangements.
4. People using care services are involved in the planning and monitoring arrangements for food service and beverage/drinks provision.
5. An environment conducive to people enjoying their meals and being able to safely consume their food and drinks is maintained (NB this can be known as ‘Protected Mealtimes’).
6. All staff/volunteers have the appropriate skills and competencies needed to ensure that the nutritional and fluid needs of people using care services are met. All staff/volunteers receive regular training in nutritional care and management.
7. Facilities and services are designed to be flexible and centred on the needs of the people using them.
8. The care-providing organisation has a policy for food service and nutritional care, which is centred on the needs of people using the service. Performance in delivering that care effectively is managed in line with local governance and regulatory frameworks.
9. Foodservice and nutritional care are provided safely.
10. Everyone working in the organisation values the contribution of people using the service and all others in the successful delivery of nutritional care.